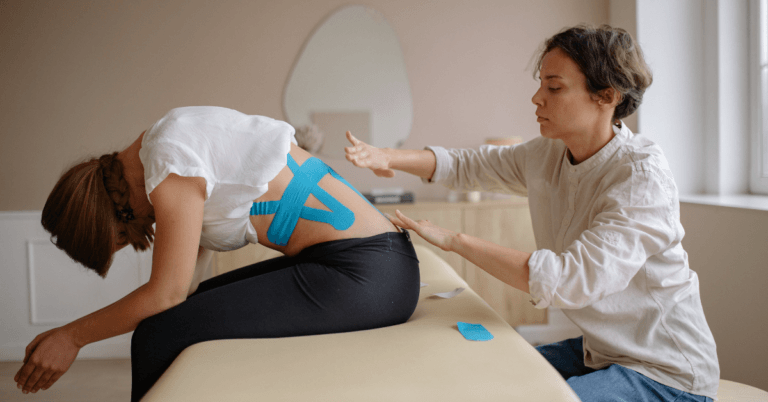
Understanding the Causes of Back Pain
Back pain is one of the most prevalent health complaints in Ireland, affecting people of all ages and activity levels. It can range from a dull, persistent ache in the lower spine to sharp, shooting sensations that radiate into the legs. Understanding why back pain develops is the first step towards finding effective, lasting relief.
The most common causes include poor posture, prolonged sitting, muscle imbalances, ligament sprains, and disc-related problems. Modern sedentary lifestyles, particularly desk-based work, place significant stress on the lumbar spine, weakening supporting muscles over time. Factors such as age, body weight, occupational demands, and previous injuries can all increase a person’s susceptibility to spinal problems.
Psychological and lifestyle factors also play a meaningful role. Stress, poor sleep, and low physical activity levels have all been linked to higher rates of chronic pain. Recognising this multi-dimensional picture is important, as effective treatment rarely involves addressing the spine in isolation.
The Different Types of Back Pain
Back pain is typically categorised as either acute or chronic. Acute back pain comes on suddenly, often following a movement, lifting injury, or awkward position, and usually resolves within a few weeks with appropriate care. Chronic pain, by contrast, persists for three months or longer and often requires a more structured rehabilitation approach.
The location of back pain also matters when determining the underlying cause. Lower back pain is the most common presentation and often involves the muscles, joints, or discs of the lumbar spine. Upper and mid-back pain, while less frequent, can be associated with poor thoracic mobility or persistent tension in the muscles surrounding the shoulder blades.
Radiating pain, where discomfort travels from the spine into the buttocks, hips, or down one or both legs, is often a sign that a nerve is involved. Conditions such as sciatica, where the sciatic nerve is compressed or irritated, require targeted physiotherapy assessment to avoid symptom escalation.
How Physiotherapy Treats Back Pain
Physiotherapy is widely regarded as one of the most effective non-surgical interventions for managing and resolving back pain. Rather than simply masking symptoms, physiotherapists aim to identify the root cause of a person’s pain and address it through hands-on treatment, movement rehabilitation, and patient education.
An initial physiotherapy assessment typically involves a detailed case history, postural analysis, range of movement testing, and orthopaedic or neurological examination as appropriate. This information guides the physiotherapist in developing an individualised treatment programme that is tailored to the patient’s specific presentation and goals.
Treatment modalities commonly used in physiotherapy for back pain include soft tissue massage, joint mobilisation, therapeutic exercise prescription, electrotherapy, and postural correction. The combination of approaches used will vary depending on the diagnosis, the acuity of symptoms, and the patient’s capacity to engage with active rehabilitation.
Spinal Decompression and Manual Therapy
For patients dealing with disc-related back pain, including herniated disc presentations, spinal decompression techniques can provide meaningful relief. Spinal decompression works by gently distracting the vertebral segments to reduce intradiscal pressure, allowing bulging or herniated disc material to retract and relieving compression on nearby nerve roots.
Manual therapy is another cornerstone of physiotherapy practice for spinal conditions. Techniques such as joint mobilisation and manipulation can restore movement to stiff or restricted spinal segments, reduce pain, and improve overall spinal function. When applied alongside an active exercise programme, manual therapy has been shown in numerous studies to produce better outcomes than either approach used in isolation.
Physiotherapists will typically reassess a patient’s response to manual therapy at regular intervals, adjusting their approach as treatment progresses. This dynamic, evidence-informed method ensures that patients receive care that is responsive to their changing needs rather than a fixed, one-size-fits-all protocol.
The Role of Dry Needling in Pain Relief
Dry needling has become an increasingly popular tool within physiotherapy practice for the management of musculoskeletal pain, including back pain. The technique involves inserting fine, sterile needles into trigger points, areas of localised muscle tightness and tenderness, to elicit a local twitch response that helps release tension and restore normal muscle function.
Unlike acupuncture, which is rooted in traditional Chinese medicine, dry needling is grounded in Western anatomical and neurophysiological principles. Research supports its use as part of a broader treatment plan for reducing pain sensitivity, improving range of motion, and promoting recovery in patients with both acute and chronic back pain conditions.
Physiotherapists trained in dry needling will always conduct a thorough assessment prior to using the technique and will discuss the procedure fully with patients beforehand. It is typically used as one component of a comprehensive treatment plan rather than a standalone intervention.
Exercises to Relieve and Prevent Back Pain
Exercise is one of the most powerful tools available for both the treatment and prevention of back pain. Physiotherapists emphasise active rehabilitation, encouraging patients to take an active role in their recovery through structured exercise programmes designed to address strength, mobility, and movement control.
Core stability exercises are commonly prescribed for back pain sufferers. Strengthening the deep stabilising muscles of the trunk, including the transversus abdominis and multifidus, helps protect the lumbar spine during daily activities and reduces the risk of recurrence. Exercises such as dead bugs, bird dogs, glute bridges, and modified planks are frequently used in clinical rehabilitation programmes.
Mobility work is equally important. Tight hip flexors, hamstrings, and a restricted thoracic spine are common contributors to lower back pain, and addressing these through targeted stretching can significantly reduce the mechanical load placed on the lumbar spine. Physiotherapists tailor exercise prescriptions to the individual’s capacity, progressing difficulty appropriately as strength and confidence improve.
Managing Sciatica and Herniated Disc Pain
Sciatica is characterised by pain, tingling, numbness, or weakness that radiates from the lower back through the buttock and down the leg, typically along the path of the sciatic nerve. It is most commonly caused by compression of a lumbar nerve root, often due to a herniated disc or bony narrowing of the spinal canal.
Physiotherapy plays a central role in the conservative management of sciatica. Depending on the presentation, treatment may include nerve mobilisation techniques, directional exercise prescription, manual therapy, and postural correction. Many cases of sciatica respond well to physiotherapy, with significant improvement often seen within six to twelve weeks when the patient engages consistently with their programme.
For those with confirmed herniated disc pathology, physiotherapy remains the recommended first-line treatment in most cases. Physiotherapists can guide patients through appropriate loading strategies that promote disc healing while managing symptoms, avoiding the need for surgical intervention in the majority of cases. Early assessment and intervention are key to achieving the best possible outcomes.
Sports Physiotherapy and Back Injuries
Athletes and active individuals are at particular risk of back injuries, with sports physiotherapy offering a specialist approach to assessment and rehabilitation in this population. Whether the injury involves a muscle strain, stress fracture, disc prolapse, or joint dysfunction, sports physiotherapists have the expertise to manage the condition while keeping return-to-sport timelines realistic and achievable.
Common sports-related back injuries include lumbar muscle strains from contact sports, stress fractures in young athletes involved in repetitive extension activities such as gymnastics or rowing, and disc injuries from heavy lifting or high-impact sport. The biomechanical demands of each sport are taken into account when designing a rehabilitation programme, ensuring patients return to activity with confidence and a reduced risk of re-injury.
Prevention is a key focus within sports physiotherapy. Identifying movement deficiencies, addressing muscle imbalances, and optimising technique are all important components of a comprehensive sports physiotherapy service. Proactive screening and pre-season conditioning programmes can significantly reduce the incidence of back injuries in sporting populations.
Preventing Back Pain in Daily Life
Prevention is always preferable to treatment, and there are many practical steps individuals can take to reduce their risk of developing back pain. Ergonomic awareness is particularly important for those who spend extended periods at a desk. Ensuring the workstation is set up correctly, with the monitor at eye level, the chair supporting the natural lumbar curve, and the keyboard positioned to allow relaxed shoulders, can make a substantial difference over time.
Regular movement breaks are essential for desk workers. Sitting for prolonged periods increases compressive load on the lumbar discs and reduces blood flow to the spinal muscles. Setting a reminder to stand and move for two to three minutes every thirty to forty-five minutes can meaningfully reduce cumulative spinal stress throughout the working day.
Lifestyle factors including maintaining a healthy weight, staying physically active, managing stress, and prioritising quality sleep all contribute to long-term spinal health. Patients who address these modifiable factors alongside their physiotherapy treatment tend to experience faster recovery and lower rates of recurrence. Building habitual physical activity into daily life, whether through walking, swimming, Pilates, or gym work, is one of the most effective strategies for a healthy spine.
When to See a Physiotherapist
Many people delay seeking professional help for back pain, hoping that symptoms will resolve on their own. While mild, short-term back pain sometimes does settle without intervention, there are clear indicators that a physiotherapy assessment is warranted sooner rather than later.
Persistent pain lasting more than two to three weeks without improvement should prompt a visit to a physiotherapist. Similarly, pain that radiates into the legs, is accompanied by numbness or tingling, significantly disrupts sleep, or follows a traumatic incident deserves prompt professional assessment. Patients with a history of osteoporosis, unexplained weight loss, or a previous cancer diagnosis should also seek assessment without delay, as back pain can occasionally signal an underlying medical condition requiring further investigation.
Red flag symptoms, including loss of bladder or bowel control, bilateral leg weakness, or saddle-area numbness, require immediate medical attention, as these may indicate cauda equina syndrome, a rare but serious spinal emergency. In all other cases, the sooner a physiotherapist can evaluate the problem, the more options are available for effective, targeted treatment. For those in the Clondalkin and wider Dublin area seeking professional support for back pain, neck pain, sciatica, or related spinal conditions, DC Physiotherapy offers evidence-based assessment and treatment from experienced practitioners who can help patients understand their condition and take meaningful steps towards recovery.